Comparison of Esophageal vs. Surface Cooling in Post-Cardiac Arrest.
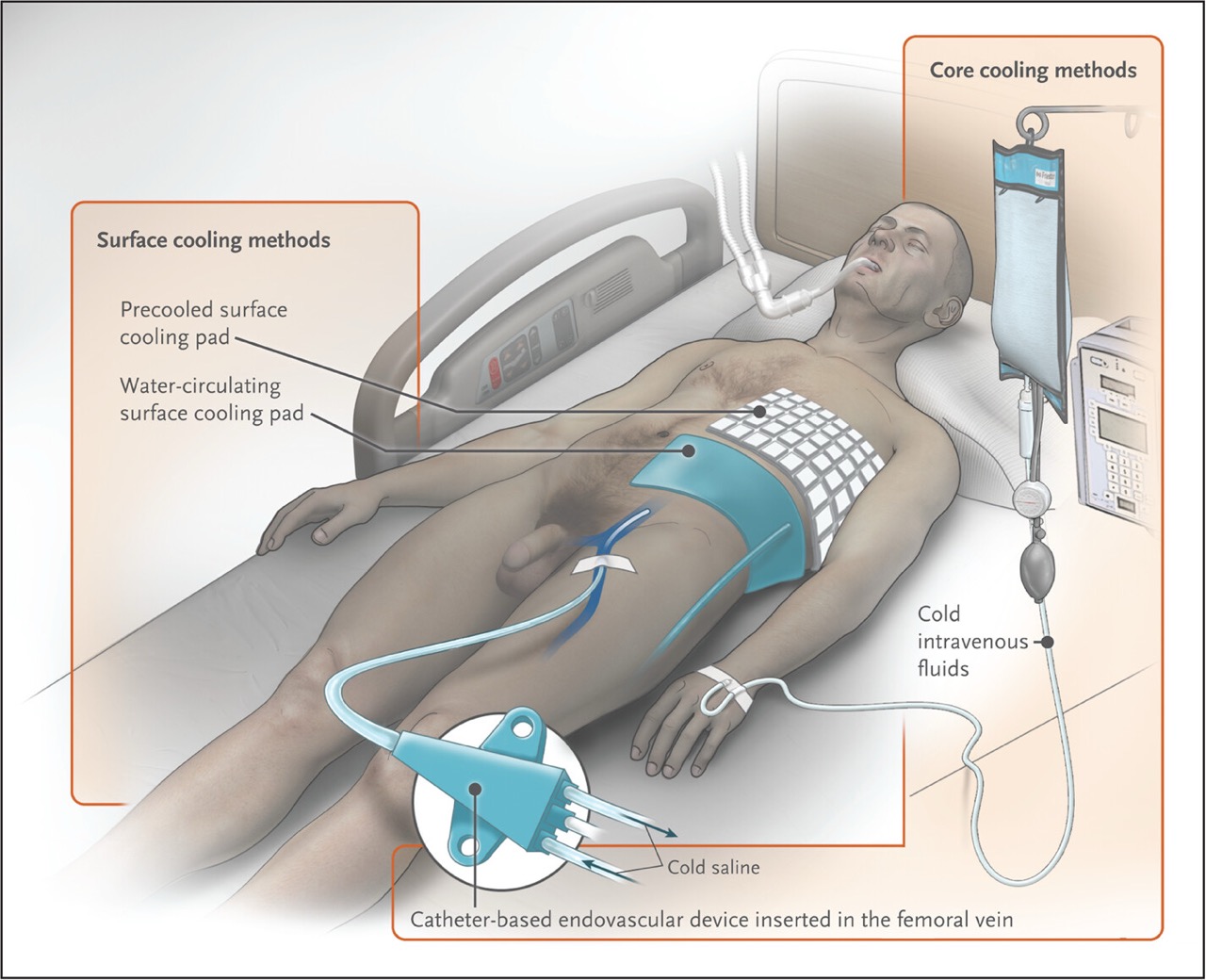
Targeted Temperature Management (TTM) is a standard of care for patients surviving out-of-hospital cardiac arrest (OHCA) to minimize neurological injury. Historically, surface cooling using ice packs or water-circulating pads has been the primary non-invasive method. However, the emergence of esophageal heat exchange technology offers a direct-to-core alternative. This research article provides a comparative analysis of esophageal versus surface cooling, evaluating thermal induction speed, maintenance stability, shivering incidence, and operational impact on the critical care team. Our findings suggest that esophageal cooling achieves significantly faster induction and superior maintenance stability without the dermatological and nursing overhead associated with surface-based systems.
Introduction
The primary goal of TTM following cardiac arrest is to maintain a constant core temperature between 32°C and 36°C to prevent secondary brain injury. While the target temperature is critical, the "precision" of reaching and maintaining that target is what often determines clinical efficacy. Surface cooling relies on conductive heat transfer through the skin and subcutaneous fat—tissues that are naturally designed to insulate the body. In contrast, esophageal cooling utilizes the high vascularity of the mediastinum. This comparison highlights the physiological and practical reasons why internal esophageal modulation is rapidly replacing external surface methods in top-tier cardiovascular centers.
Induction Speed: The Race to Target Temperature
In the context of post-cardiac arrest care, time is brain. The speed at which a patient reaches the target temperature is a key performance indicator for ICU teams.
- Surface Cooling Limitations: Surface pads must overcome the "insulation barrier" of the skin and body fat. In patients with high Body Mass Index (BMI), surface cooling is notoriously slow and often fails to reach target temperatures within the recommended window. Furthermore, peripheral vasoconstriction caused by cold skin can actually trap heat in the core, a phenomenon known as the "insulation effect."
- Esophageal Induction: Because the esophageal device is placed internally, it bypasses the skin and fat entirely. It transfers heat directly to the blood flowing through the aorta and the heart. Clinical data indicates that esophageal cooling can achieve target temperatures up to 2.5 times faster than traditional surface blankets, particularly in patients where external surface area is limited or body mass is a factor.
Maintenance Phase: Stability vs. Fluctuations
Once the target temperature is reached, the "maintenance phase" begins. This phase requires precise, constant modulation to prevent temperature "drifting."
- Surface Cooling: Surface systems often struggle with "overshoot" (cooling the patient too much) and "undershoot" (allowing the temperature to rise). This results in a "sawtooth" temperature graph, which can trigger inflammatory responses in the brain.
- Esophageal Stability: The high-flow, closed-loop nature of esophageal devices allows for much tighter control. By interacting directly with the thermal core, the system can make minute adjustments to the water temperature to keep the patient within ±0.1°C of the set point. This level of stability is nearly impossible to achieve with external pads that are influenced by ambient room temperature and patient blankets.
Shivering and Metabolic Stress
Shivering is one of the most significant complications of TTM. It increases metabolic rate, oxygen consumption, and intracranial pressure—all of which are detrimental to a recovering cardiac arrest patient.
- Skin vs. Core: Shivering is primarily triggered by skin thermoreceptors. When cold pads are applied to the skin, the body perceives a massive thermal threat and initiates a vigorous shivering response.
- Esophageal Advantage: Esophageal cooling focuses on the core. Because the skin remains warm and accessible, the cutaneous thermoreceptors are not stimulated in the same way. Studies have shown a significant reduction in the "Bedside Shivering Assessment Scale" (BSAS) scores when using esophageal methods, which leads to a decreased need for heavy sedation and paralytics.
Operational and Nursing Impact
The choice between surface and esophageal cooling has profound implications for the nursing staff and the overall management of the patient’s environment.
Skin Integrity and Wound Care
Surface cooling pads cover up to 70% of a patient’s body surface area. This creates a moist, cold environment that is highly conducive to skin breakdown and pressure ulcers. Nurses are often unable to perform required skin assessments without pausing the cooling therapy. Esophageal cooling leaves the skin entirely clear, allowing for:
- Standardized turning and repositioning.
- Continuous monitoring of surgical sites or IV access points.
- Improved hygiene and wound management.
Patient Access and Diagnostic Mobility
A patient covered in cooling pads and hoses is difficult to move. If a post-cardiac arrest patient needs an emergency CT scan or a trip to the catheterization lab, surface pads must often be disconnected or repositioned, causing a loss of thermal control. The esophageal device, being internal and compact, travels with the patient effortlessly. Its radiolucent design ensures it does not interfere with life-saving imaging, providing uninterrupted TTM throughout the entire continuum of care.
Cost-Effectiveness and Resource Allocation
While the initial cost of single-use esophageal devices is a factor, the long-term health economics often favor this method. Reduced nursing labor, lower sedation requirements, and the prevention of hospital-acquired pressure ulcers (HAPUs) contribute to a lower total cost per patient stay compared to the expensive water-circulating surface systems that require constant monitoring and expensive replacement pads.
Conclusion
When comparing esophageal versus surface cooling in the post-cardiac arrest population, the data favors the esophageal approach in nearly every clinical category. From faster induction times and tighter maintenance stability to the preservation of skin integrity and reduced shivering, esophageal heat exchange technology provides a superior clinical experience for both the patient and the healthcare provider. As the "New Era" of TTM continues to unfold, the transition from external surface methods to direct-to-core esophageal modulation represents a significant advancement in the pursuit of improved neurological outcomes.

